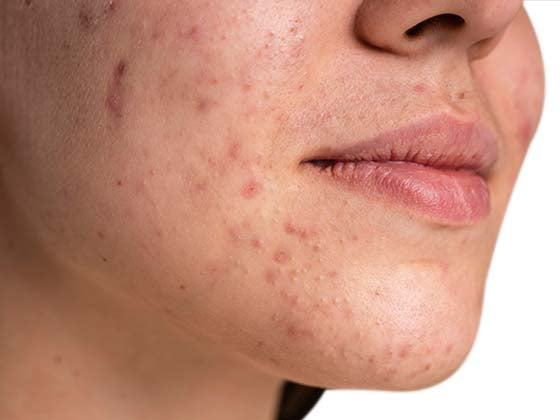
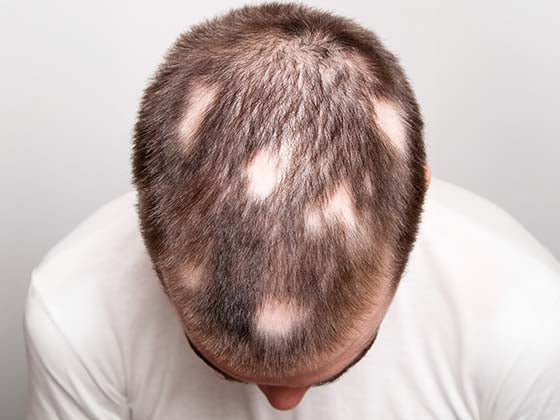
Shingles, caused by the varicella-zoster virus (VZV), is a painful rash that usually affects one side of the body. In this article, we will discuss several triggers and prevention methods for shingles activation.
What is Shingles?

Shingles, commonly known as herpes zoster, is a viral infection caused by the varicella-zoster virus (VZV), which causes chickenpox. After a person has experienced chickenpox, VZV remains dormant in their neurological system. Later in life, typically many years after the initial infection, the virus might reactivate and produce shingles.
Overview of Shingles
Shingles is a viral illness that leads to a painful rash. Shingles can arise anywhere on the body. Typically, it appears as a single stripe of blisters wrapping across the left or right side of your body. Shingles is caused by the varicella-zoster virus, which also causes chickenpox. After having chickenpox, the virus remains in your body for the rest of your life. Years later, the virus may resurface, resulting in shingles.
Shingles are not life-threatening. But it can be uncomfortable. Vaccines can reduce the risk of shingles. Early therapy can shorten a shingles infection and reduce the risk of complications. The most prevalent consequence is postherpetic neuralgia. This is a painful disorder that produces shingles agony even after the blisters have healed.
The Role of the Varicella-Zoster Virus

The varicella-zoster virus (VZV) is a major cause of two separate human illnesses: chickenpox (varicella) and shingles. Here's a summary of its function and how it manifests in certain conditions:
Chickenpox (Varicella)
-
VZV is primarily transmitted via respiratory droplets or direct contact with fluid from infected patients' blisters.
-
VZV produces chickenpox when infected for the first time, which usually occurs in childhood. Symptoms include a typical itchy rash that begins on the face and trunk and extends to the rest of the body, as well as fever and fatigue. The virus replicates in the respiratory tract before spreading to the skin, resulting in the characteristic blisters.
-
After recovery, the immune system normally eliminates the virus, but some VZV stays dormant in nerve tissues.
Shingles (Herpes Zoster)
-
VZV can stay dormant in the neurological system for decades after the first chickenpox infection. Aging, stress, and reduced immune function can all contribute to viral reactivation. Reactivation enables the virus to migrate to the skin via nerve fibres, resulting in the painful rash known as shingles.
-
Shingles usually manifests as a painful, unilateral rash that looks like a band or stripe of blisters on one side of the body or face. Pain, itching, burning, and sensitivity to touch may occur before the rash.
-
Shingles can cause consequences such as postherpetic neuralgia (lasting pain after the rash has healed), bacterial skin infections, and, in rare cases, neurological issues if the virus damages the nerves.
Understanding Shingles Symptoms
Shingles, commonly known as herpes zoster, has various unique symptoms. Here's a thorough list of shingles symptoms, including pain, burning, or tingling sensations, localized rash, blisters, itching, and other symptoms (including fever, headache, and fatigue).
Common Triggers of Shingles Activation

Shingles are caused by the reactivation of the varicella-zoster virus (VZV), which can be triggered by a variety of conditions that weaken the immune system or impair the body's ability to keep the virus dormant. Here are some frequent causes of shingles activation:
-
Age: As one becomes older, the risk of developing shingles increases significantly. As people age, especially those over the age of 50, their immune systems may deteriorate, making them more vulnerable to VZV reactivation.
-
Weakened Immune System: Conditions or treatments that weaken the immune system increase the likelihood of developing shingles. These include HIV/AIDS and other disorders that weaken the immune system. Cancer treatments include chemotherapy and radiation. Immunosuppressive drugs are used following organ transplantation.
-
Stress: Physical or emotional stress can weaken the immune system, making it more difficult for the body to suppress VZV reactivation.
-
Underlying Medical Conditions: Chronic disorders like diabetes and autoimmune diseases might compromise immune function, increasing the risk of shingles.
-
Medications: Certain medications, such as steroids or prolonged use of antibiotics, can suppress the immune system and contribute to VZV reactivation.
-
Trauma or Injury: Physical trauma or injury to a specific area of the body can sometimes trigger shingles in that dermatome (area of skin supplied by a single spinal nerve).
-
Previous Chickenpox Infection: Having chickenpox in the past makes VZV inactive in nerve tissues. Later in life, circumstances that impair the immune system can cause the virus to return to shingles.
Impact of Weakened Immune System

A compromised immune system can have serious consequences for overall health and susceptibility to a variety of illnesses and disorders. Some important features of how a weaker immune system can affect people include increased susceptibility to infections (such as viral, bacterial, and fungal infections), impaired wound healing, chronic health conditions, an increased risk of cancer, and an impact on vaccination. Understanding the impact of a compromised immune system emphasizes the necessity of medical intervention, preventive measures, and continuous healthcare assistance in improving health outcomes and quality of life for afflicted people.
Stress as a Catalyst for Shingles
Recognizing the relationship between stress and shingles activation emphasizes the need for stress management to preserve general health and lower the likelihood of disease reactivation. Individuals who adopt healthy living choices and use stress reduction techniques can enhance their immune systems and potentially reduce the incidence of shingles outbreaks.
Other Risk Factors for Shingles

Aside from stress and a weaker immune system, several other risk factors can increase the likelihood of having shingles. These factors may lead to the reactivation of the varicella-zoster virus (VZV) and the development of shingles symptoms. Other significant risk factors include age, a history of chickenpox, medical conditions and treatments, medications, stress and emotional variables, ethnicity and genetics, gender, and localized factors. Early detection and effective medical therapy are critical for minimizing the problems associated with shingles outbreaks.
Prevention and Management of Shingles

Shingles prevention and treatment approaches include ways to reduce the chance of contracting the disease and treat symptoms if an outbreak does occur. Here are the primary techniques to prevention and management:
Prevention
-
The shingles vaccination (Shingrix) is extremely successful in lowering the risk of shingles and associated consequences. It is indicated for individuals aged 50 and more, including those who have already had shingles or had the earlier vaccination (Zostavax). Vaccination not only lowers the risk of developing shingles, but it also lowers the risk of postherpetic neuralgia (pain that persists after the shingles rash has healed) and other problems.
-
Maintain a nutritious diet high in fruits, vegetables, and whole grains to boost immunological function. Regular physical activity can help relieve stress and boost the immune system.
-
Use stress-reduction practices including yoga, meditation, deep breathing exercises, and mindfulness. Avoid excessive stress, and seek help from friends, family, or a counselor if necessary.
-
Practicing excellent hygiene, such as frequent handwashing, can help prevent the spread of VZV to others who are susceptible to chickenpox or have not received the shingles vaccine.
Management
-
If you suspect you have shingles or have symptoms such as pain, tingling, or a rash, seek medical assistance right once. Antiviral drugs, such as acyclovir, valacyclovir, or famciclovir, can help reduce the intensity and duration of shingles if used within 72 hours of the rash appearing.
-
Acetaminophen (paracetamol) and nonsteroidal anti-inflammatory medications (NSAIDs) are two over-the-counter pain medicines that can aid with the pain and discomfort caused by shingles. Topical therapies containing capsaicin or lidocaine may alleviate localized pain.
-
Keep the rash clean and dry to avoid bacterial infection. Cool compresses or oatmeal baths might help relieve itching and pain.
-
To avoid long-term discomfort, rapidly manage and treat problems such as postherpetic neuralgia. Watch for evidence of bacterial infection in the rash and seek medical assistance if symptoms worsen or do not improve.
Importance of Shingles Vaccination

Shingles immunization is important for preventing shingles, lowering disease severity if it does develop, and avoiding consequences such as postherpetic neuralgia. It provides a safe and effective approach to protect people aged 50 and up against the effects of shingles, contributing to overall public health efforts to minimize the burden of VZV-related disorders. Individuals should consult with their healthcare physician to decide the best timing and schedule for immunization, taking into account the advantages and recommendations.
Tips for Strengthening the Immune System

Strengthening the immune system is critical for overall health and well-being as it allows the body to fight infections and function optimally. Here are some effective ways to enhance and maintain a healthy immune system:
-
Eat a Balanced Diet: Consume a wide range of fruits, vegetables, whole grains, lean proteins (such as chicken, fish, beans, and nuts), and healthy fats. Drink enough amounts of immune-boosting nutrients such as vitamin C (found in citrus fruits and bell peppers), vitamin D (from sunlight and fortified meals), zinc (found in meat, shellfish, nuts, and seeds), and antioxidants.
-
Get Regular Exercise: Engage in at least 150 minutes of moderate-intensity activity per week, such as brisk walking, running, cycling, or swimming. Exercise improves circulation, lowers inflammation, and boosts immunological function.
-
Get Sufficient Sleep: Aim for 7-9 hours of sleep each night. Quality sleep improves immune function, facilitates recuperation, and regulates hormones that affect immunity.
-
Manage Stress: Engage in stress-relieving activities such as mindfulness meditation, deep breathing exercises, yoga, or spending time outside. Chronic stress can impair the immune system, so developing good stress-management strategies is important.
-
Stay Hydrated: Stay hydrated throughout the day to promote general health and the appropriate function of immune cells and organs.
-
Maintain a Healthy Weight: Aim for a healthy body weight by eating a well-balanced diet and exercising regularly. Obesity can weaken the immune system and increase vulnerability to infections.
-
Practice Good Hygiene: Wash your hands frequently with soap and water, especially before eating, after using the lavatory, or while in contact with potentially contaminated surfaces. To lessen the risk of infection, limit your exposure to sick or contagious individuals.
-
Quit Smoking and Limit Alcohol: If you smoke, you should consider stopping. Smoking affects the immune system, raising the risk of respiratory infections and other ailments. Limit your alcohol consumption, as it can affect immune function and overall health.
-
Consider vitamins: If necessary, consider taking immune-boosting vitamins like vitamin C, vitamin D, zinc, or probiotics. Before using any new supplements, consult with your doctor.
-
Vaccinations: Follow the recommended vaccination schedule, which includes the flu vaccine as well as shots for preventable diseases like measles, mumps, rubella, and pneumonia.
Managing Stress to Prevent Shingles
Effective stress management can help reduce the incidence of shingles (herpes zoster) outbreaks because stress weakens the immune system and contributes to the reactivation of the varicella-zoster virus (VZV). Stress reduction approaches, physical activity, healthy living habits, social support, time management, mind-body practices, and limiting stressful triggers are all useful stress management tactics for shingles prevention. By adopting these stress management practices into your daily routine, you can lessen the effects of stress on your immune system and overall health. This, in turn, may help reduce the incidence of shingles breakouts while also supporting your body's capacity to maintain normal immunological function and resistance to infections.
Living with Shingles: Coping Strategies

Living with shingles can be difficult owing to the pain and potential problems linked with the condition. Here are some coping tactics for managing and alleviating symptoms during a shingles outbreak:
-
Medical Treatment: Take the antiviral drugs provided by your doctor to help lessen the severity and duration of the shingles rash and its complications. To treat pain and suffering caused by the rash, take over-the-counter pain medications like paracetamol or nonsteroidal anti-inflammatory medicines (NSAIDs). To relieve itching and pain, apply topical creams or lotions containing capsaicin or lidocaine directly on the rash.
-
Skin Care: Gently wash the rash with mild soap and water, then pat dry with a soft cloth. Avoid rubbing or aggravating the affected region. To reduce rash irritation, wear loose, soft clothing. Avoid using strong cleansers, fragrances, or chemicals on the affected skin.
-
Pain Management: Apply cool, damp compresses or take cool baths with colloidal oatmeal to relieve itching and discomfort. Use soft pillows or cushions to support areas affected by shingles, especially if the rash is on the torso or other sensitive areas.
-
Rest and Recovery: Allow yourself enough rest and avoid strenuous activities that may aggravate pain or discomfort. Deep breathing, meditation, and listening to peaceful music are all stress-reduction practices that can help you relax and heal.
-
Nutrition and Hydration: Drink plenty of water and fluids to stay hydrated and promote overall healing and skin health. Consume a well-balanced diet high in vitamins, minerals, and antioxidants to boost immune function and help healing.
-
Monitor for Complications: Monitor the rash for symptoms of infection, such as increased redness, swelling, warmth, or pus. If you detect any worrying symptoms, please contact your healthcare professional.
-
Emotional Support: Lean on friends, family, or support groups for emotional support and encouragement as you recover from shingles. If required, consult with a counselor or therapist to help you cope with the emotional effects of shingles and successfully manage stress.
-
Follow-up Care: Follow your doctor's recommendations for medication, wound care, and follow-up appointments to track your progress and avoid complications.
Effective Shingles Treatment Options
Early intervention with antiviral medications, pain management measures, and supportive care are essential for promoting healing and reducing the risk of complications with shingles. Prompt medical attention and commitment to treatment instructions are critical for successfully controlling shingles and minimizing their impact on daily life.
Pain Management for Shingles

Effective shingles pain management frequently entails a combination of drugs, topical treatments, and supportive therapy suited to each patient's specific needs. Early intervention and thorough care can help to reduce discomfort, enhance healing, and improve general health during and after a shingles outbreak. Consult your healthcare physician for personalized recommendations and guidance on how to manage shingles-related pain.
Preventing Shingles Complications
Preventing shingles (herpes zoster) consequences requires early detection of symptoms, timely medical action, and thorough care measures. Key actions to prevent sequelae include vaccination, early medical intervention, skin care, and hygiene, eye care (if impacted), managing postherpetic neuralgia (PHN), monitoring and follow-up, maintaining overall health, and avoiding high-risk situations. Individuals can dramatically minimize their risk of shingles-related problems by implementing preventative measures such as immunization, early medical intervention, adequate skin care, and monitoring for complications such as PHN. Prompt consultation with healthcare specialists is critical for personalized guidance and timely symptom management to avoid long-term complications linked with shingles outbreaks.
Seeking Medical Advice: When to Consult a Doctor

If you have shingles symptoms or suspect you have been exposed to the virus, visit a doctor right away. Shingles symptoms, eye involvement, a weakened immune system, severe pain or problems, pregnancy, vaccine concerns, and general worries are all essential reasons to seek medical attention. It is crucial not to postpone seeking medical assistance, especially if you are having symptoms of shingles or related problems.